Home » Sleep
Sleep
Approximately half of all adult men and a third of all women snore. Not only is it a sign of sleep apnea, but it can also lead to daytime fatigue and relationship problems. If your partner keeps telling you that you snore, make an appointment with the experts at Lakeshore Ear, Nose & Throat Center in St. Clair Shores, Macomb Township, Rochester, Grosse Pointe, and Sterling Heights, Michigan. For help with your snoring or sleep apnea, call or schedule a consultation online today.
What causes snoring?
Snoring is the result of vibrations in the uvula and soft palate at the back of your throat when you sleep. The vibrations are caused by your breath moving those soft tissues on both your inhale and exhale.
There are several contributing factors that may cause you to snore, including:
- Structural abnormality or weakness in the base of the tongue, tonsils, and soft palate
- Excess weight or obesity
- Nasal or sinus problems
- Age
- Use of sedatives or alcohol
A sleep disorder known as sleep apnea may also be responsible for your snoring.
At Lakeshore ENT, we understand that one size does not fit all when it comes to sleep apnea solutions. Dr. Daniel D. Martin is proud to offer Inspire therapy as an implantable treatment option for people with Obstructive Sleep Apnea who are unable to use or get consistent benefits from CPAP.
What is Inspire for Sleep Apnea?
Inspire is an innovative sleep apnea treatment designed to provide a breath of fresh air to those who struggle with traditional CPAP therapy. This implantable device works with your body’s natural breathing process, delivering a personalized solution to keep your airway open during sleep.
How does it work?
Controlled by a compact handheld sleep remote, you can activate Inspire therapy before bedtime and deactivate it upon waking up. Inspire monitors your breathing patterns while you are asleep, and the system delivers mild stimulation to the hypoglossal nerve, which controls the movement of your tongue and other airway muscles. By stimulating these muscles, the airway remains open during sleep.
Additionally, you have the flexibility to adjust stimulation strength, both increasing and decreasing it and pause the therapy during the night if necessary.
Is Inspire safe?
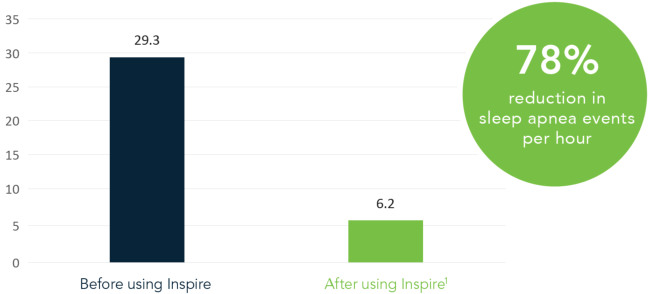
The safety and effectiveness of Inspire therapy have been measured in over 100 peer-reviewed articles. Studies show patients using Inspire therapy experience significant reductions in sleep apnea events, increased daytime activity levels, and reduced daytime sleepiness.
Inspire therapy is safe, clinically proven, and FDA-approved.
If you’re ready to increase your sleep quality, request an appointment, today.