Home » Pediatric ENT Treatments
Pediatric ENT Treatments
When your child gets an ear infection or has chronic tonsillitis and the accompanying sore throats it causes, you need a pediatric ENT who can help your child recover quickly. The specialists at Lakeshore Ear, Nose & Throat Center provide expert medical care and compassionate attention for kids and their families in the communities north of Detroit, including St. Clair Shores, Macomb Township, Rochester, Grosse Pointe, and Sterling Heights, Michigan. Call or schedule an appointment online today to learn more.
How is pediatric ENT care different from ENT care for adults?
Children have different ENT needs than adults. First, they are physiologically different, and smaller, more delicate tools are needed to examine and treat your child. Also, children usually develop different ENT conditions than adults.
Your pediatric ENT specialist at Lakeshore has completed additional specialized training, which helps them make your child feel comfortable during examinations and treatments. They can also diagnose conditions even if your child doesn’t have the speech skills or vocabulary to describe their symptoms the way an adult would.
What are common pediatric ENT conditions?
While most ENT conditions occur in both pediatric and adult patients, many are more common among children, such as:
- Ear infections
- Tonsillitis and enlarged adenoids
- Sore throats and hoarseness
- Breathing difficulties
- Nosebleeds
- Foreign objects in the ear, nose, or throat
- Hearing loss
- Congenital abnormalities
The providers at Lakeshore ENT are experts at determining the cause of your child’s condition regardless of their age.
What causes ear infections?
Most ear infections develop in the middle ear, or the eustachian tubes, behind the eardrum. Ear infections develop when bacteria or a virus gets into the middle ear and causes an inflammatory response, and the tube fills with fluid or pus.
If your child has an ear infection, they’ll typically develop a fever and complain of pain either verbally or by tugging or rubbing their ear. Ear infections can cause trouble eating, drinking, or sleeping by changing the pressure in the ear.
Children are more likely to get ear infections because their eustachian tubes are shorter and more horizontal at this stage of physical development, which increases the chance of bacteria and viruses reaching the middle ear.
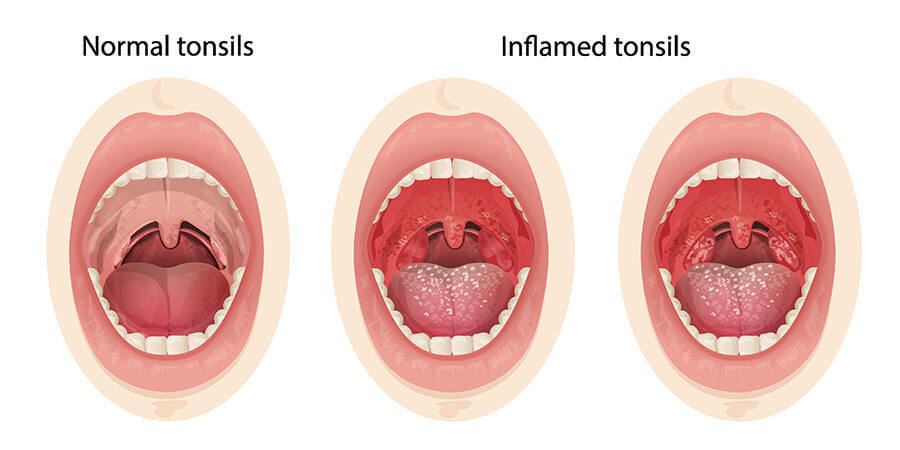
What are signs that my child needs their tonsils removed?
Frequent, recurring throat infections, like tonsillitis or strep throat, are the primary sign that your child might need a tonsillectomy (tonsil removal).
Your child may also need their tonsils removed if their tonsils and adenoids are so enlarged that it disrupts their breathing.
The tonsils and adenoids are lumps of tissue on the sides of the throat that help fight infections by reducing the chances of bacteria or viruses traveling down the throat to the lungs or digestive tract. Sleep apnea and snoring are signs of oversized tonsils and adenoids in children.
The Lakeshore pediatric ENT specialists provide comprehensive care for children and their families and only recommend surgery when it is the best option to improve and protect your child’s health.
If you’re concerned your child may have an ear, nose, or throat issue, call or make an appointment online to meet with the pediatric specialists at Lakeshore Ear, Nose & Throat Center.